The American Opioid Epidemic
by Taylor Walker
This study examines the medical, legal, and socioeconomic problems underlying the ongoing opioid epidemic in America with emphasis on finding effective policy solutions. In the medical system, a lack of oversight of pharmaceutical companies, deceptive marketing practices used by pharmaceutical companies targeting doctors, a massive increase in opioid production and sales, and the industrialization and automation of the medical profession are all major factors that contribute to the epidemic. The legal system contributes to the epidemic through its punitive stance towards drug use/abuse that has persisted since the 1970s which caused a massive increase in the incarcerated population and corrections spending. Additionally, the little training police officers receive concerning substance abuse, and the lack of access to rehabilitation and treatment programs in prisons also contribute to this epidemic. Socioeconomic problems relate to the lack of community-based programs for those at highest risk of addiction, and those programs have been underfunded and understaffed for decades. This paper concludes with several policy reform suggestions for our medical and legal systems. Overall, this study suggests that adopting a less punitive stance towards the epidemic, and, instead, addressing it as a public health problem would help curtail the ever-increasing death toll and bring an end to the epidemic.
America is currently facing an unprecedented epidemic of opioid abuse. This epidemic is mainly due to the fact that for the past few decades opioids have flooded onto America’s streets. However, many of these drugs have not come from the shady hands of drug dealers but rather from the trusted hands of medical professionals. Additionally, the sheer number of opioids involved in this epidemic is astounding with most of the them having come from the labs of pharmaceutical companies rather than the labs of drug traffickers (Lembke, 2016). These drugs are on America’s streets mainly due to the efforts of pharmaceutical companies promoting the liberal use of prescription opioids. These efforts have resulted in a massive increase of prescription opioid addictions in America.
Pharmaceutical companies, however, are not the only ones to blame. Since the beginning of Nixon’s War on Drugs, convictions for drug users have skyrocketed, and the length of sentences for drug possession have increased dramatically (Clear and Frost, 2014). Due to this, thousands of drug addicts are now locked up and look forward to decades of incarceration. Additionally, few prisoners receive treatment for their addiction due to the lack of funds for prisoner rehabilitation (Clear and Frost, 2014). Moreover, once released, former prisoners are banned from using social welfare services such as food stamps and public housing. These services are key for not only former prisoners but also the lower class because these services help fight addiction. Given the fact that many prisoners and drug addicts come from lower socioeconomic classes, this ban only exacerbates their problems, and encourages them to return to breaking the law (Clear and Frost, 2014). The legal policies currently in place have contributed to this epidemic by wasting millions of taxpayer dollars on ineffective programs that have done little to discourage drug use. Overall, the goal of this paper is to shed light on the problems that have caused this epidemic, and to promote policies that will curb it. Therefore, I highlight the systemic problems in our medical, legal, and socioeconomic systems that contribute to this epidemic, and I will also offer solutions that policymakers could enact to control this epidemic.
The Current Epidemic
The current epidemic is quite different than those that have occurred in the past. Generally, past epidemics have been shorter, and did not involve that many Americans. For example, in the early 1900s, America faced a heroin epidemic that was similar to our current epidemic. However, it was quickly suppressed by the Narcotics Tax Act of 1914 which banned physicians from prescribing opioids (Alam and Jurrlink, 2016). While this law took care of the supply of opioids, economic reforms in the 1920s and 1930s helped decrease demand of opioids, and prevented a rebound in opiate use (Jones, 1995).
Currently, there are 2.4 million Americans suffering from severe opioid use disorder (Vashishtha, Mittal, and Werb, 2017). Additionally, opioid overdoses have substantially increased over the past decade. For example, Figure 1 shows that in 2002 opioids caused around 12,000 overdose deaths, but in 2015 opioids caused almost 35,000 overdose deaths. This means that opioid overdose deaths have almost tripled within the past few years. Further compounding this epidemic is the fact that physicians are prescribing more opioids for chronic pain, resulting in prescription opioid sales quadrupling since 1999 (Reinl, 2017). Lastly, this epidemic costs the US almost $128.2 billion dollars per year, and has affected every demographic in the US regardless of wealth, race, or location (Clarke, Skoufalos, and Scranton, 2016). Simply put, most of these statistics are due to the shortcomings and policies of America’s medical, legal, and socioeconomic systems which will be addressed in the following sections.

Figure 1. National Institute on Drug Abuse. This figure shows the rapid increase in opioid related deaths from 2002 to 2015. From 2002 to 2015, opioid related deaths tripled from 10,000 to 35,000.
Systemic Problems Underlying the Opioid Epidemic
Medical Problems
The largest contributor to this epidemic are the systemic problems in the medical field. These problems have mainly come about due to the high number of prescription opiates handed out each year. Two hundred and seven million opioid prescriptions were handed out in 2013, while only 76 million were written in 1991 (Kanouse and Compton, 2015). This shows that prescriptions for opioids have doubled within the past two decades. Additionally, opioid sales have also increased. Between 1999 and 2010, prescription opioid sales and prescription opioid usage quadrupled (Manchikanti et al., 2012). Americans consume about 80% of the world’s prescription opioids, and, in 2007, prescription opioids were the second most abused drug in America (Manchikanti et al., 2012). Along with the increase in opioid usage, the number of emergency room visits and overdose deaths also increased. From 2004 to 2008, emergency room visits related to prescription opioid abuse rose by 105% (Kanouse and Compton, 2015). Additionally, almost 50% of all drug-related emergency room visits are due to drug abuse, and opioids are the second most commonly abused drug involved in those visits (Kanouse and Compton, 2015). Finally, these increases in usage have culminated in the significant rise of opioid overdoses. Currently, prescription opioids cause about 1 death every 36 minutes in America (Manchikanti et al., 2012). Additionally, in 2010, 57.7% of the 38,329 overdose deaths involved opiates (Kanouse and Compton, 2015). Today’s doctors not only have to contend with fighting opiate addiction but also preventing opiate overdoses.
The explosive growth of opioid sales is mainly due to the influence of pharmaceutical companies. The best example of the massive amount of influence pharmaceutical companies have in the medical community is the production and marketing of Oxycontin. In the early 2000s, there were allegations within the medical community that companies falsely marketed commonly prescribed opioids, such as Oxycontin, as having a reduced risk of addiction (Kanouse and Compton, 2015). These companies also marketed their product to physicians by distributing coupons and releasing promotional videos which falsely claimed an addiction rate of less than 1% (Kanouse and Compton, 2015). By directly advertising to physicians, these companies were able to dramatically increase their sales even though they knew some of the information they distributed was false. These companies eventually admitted to the false marketing allegations. Purdue Pharmaceuticals had to pay a fine of $634 million dollars for misbranding Oxycontin (Lembke, 2016). These companies responded to the allegations by coming up with derivatives of Oxycontin which were specifically designed to prevent abuse (Kanouse and Compton, 2015). However, these derivatives have also contributed to the opioid epidemic in the same way Oxycontin did (Kanouse and Compton, 2015). Sadly, instead of taking the initiative to try and curb the opioid epidemic, it seems that pharmaceutical companies have tried to capitalize off of it.
Further perpetuating this epidemic is the changing nature of practicing medicine in the US. Over the past few years, the medical field has become industrialized and automated which has resulted in doctors being left with very little agency (Lembke, 2016). The medical expertise of doctors has been usurped by the financial motives of hospital administrators and insurance agents, and this has been very detrimental to the health of patients (Lembke, 2016). Due to these changes, doctors are concerned about whether they are meeting the billing quotas set by their employer (Lembke, 2016). As a result, doctors have little time to determine if a patient is abusing opioids and have even less time to assist patients who are abusing opioids (Lembke, 2016). Doctors have become increasingly overburdened in the past few years, and these regulations and quotas have only made matters worse. Unless the medical field changes, doctors will not be able to properly combat this epidemic.
Legal Problems
Throughout the past few decades, America’s legal policies have reflected a change in how our system views criminals, and, consequently, drug offenders. Criminals have gone from citizens who can be rehabilitated to citizens who should be indefinitely locked up and harshly punished (Clear and Frost, 2014). Going along with this shift, the causes of crime have also changed. Before Nixon, crime was thought of as a byproduct of society and criminality was due to societal ills such as unemployment, poverty, and economic inequality (Clear and Frost, 2014). However, Nixon helped shift public opinion on the origins of crime due to a crime wave that occurred during that time. Crime became an individual act caused by individual factors, and public policy changed accordingly by inflicting harsher sentences on offenders (Clear and Frost, 2014). By shaping public opinion, policymakers were able to portray criminals as degenerates whose only purpose was to cause disorder in society. This dehumanization of criminals has extended to drug addicts as well, causing us to view them the same way we view criminals. Moreover, the implied solution to this epidemic was not to rehabilitate offenders but rather to enforce harsher punishments on criminals (Clear and Frost, 2014). This shift has manifested in the form of harsher sentences for criminals through policies such as three-strikes laws and mandatory minimums and has especially affected drug offenders who are being grouped together with criminals of more serious crimes.
The end result of these policies is sentences that can span years for citizens who have committed petty drug crimes, such as possession. Furthermore, these policies have resulted in an explosive growth of prisoners who are incarcerated for drug crimes (The Sentencing Project, 2017). Figure 2 indicates that in 1980 only 4,789 people were incarcerated in federal prison due to drug offenses, but in 2015 that number grew to around 92,000 people (Figure 2 and Figure 3). Likewise, in 1980, state prisons had around 19,000 people incarcerated due to drug offenses. By 2015, that number had risen to over 206,000 people (Figure 2). Moreover, Figure 3 shows that drug offenders incarcerated in federal prisons have increased at a steady rate since 1980. It also shows that drug offenders have made up almost 50% of the federal prison system’s population since 1990 (Figure 3). Additionally, the large increase in the prison population was also accompanied by a large increase in spending. In 2014, America spent $70 billion dollars on its correctional system while in 1982 America only spent $10 billion dollars; simply put, America’s correctional budget increased by over 660% since 1982 (Clear and Frost, 2014). Overall, the implementation of punitive policies that target drug abusers has been very costly and has had a profound effect on the number of drug users who go to prison.
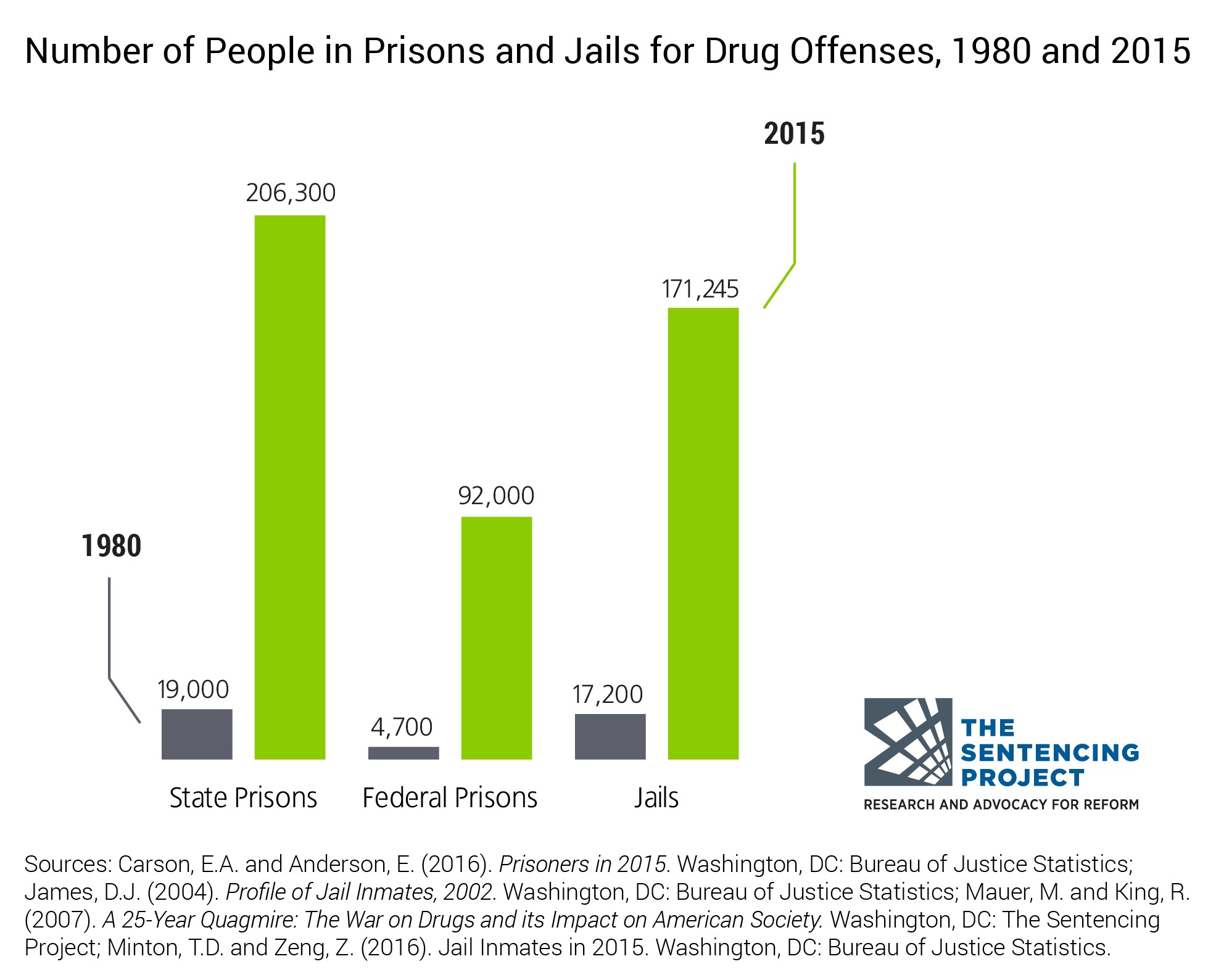
Figure 2. The Sentencing Project. This figure shows the large increase in offenders who were incarcerated for drug offenses from 1980 to 2015. Note that drug offenders are predominantly incarcerated at the state and local level, and that drug offenders account for almost 500,000 prisoners in our correctional system.
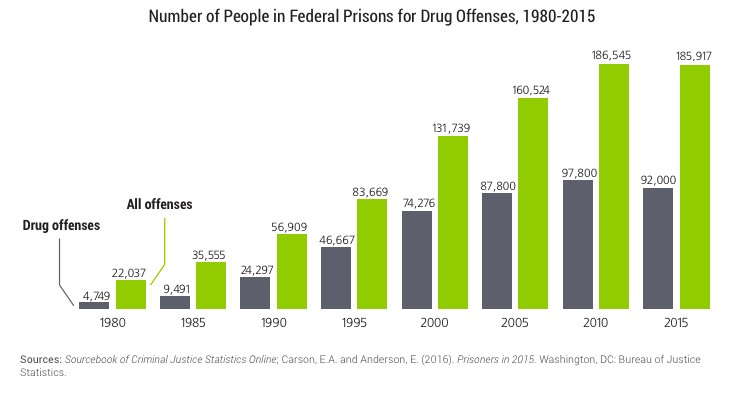
Figure 3. The Sentencing Project. This graph shows the rise of incarcerated drug offenders in the federal prison system. Note that since 1990 half of all prisoners in the federal system were incarcerated due to drug offenses.
The shift from rehabilitative policies to punitive policies has also come at the cost of rehabilitation programs. Even though corrections spending has increased over the past few decades, there has been a significant decline in funding for rehabilitation programs. This is mainly due to the fact that 90% of corrections spending goes towards maintaining prisoner incarceration and leaves very little funds for rehabilitation (Clear and Frost, 2014). These spending practices are maintained even though treatment programs have been shown to significantly reduce the chances of recidivism and addiction relapse, and the successful implementation of these programs would reduce the overall cost of incarceration in the criminal justice system (Zarkin et al., 2012). Since almost 53% of prisoners meet the diagnostic criteria for substance use disorder, these programs would be very effective and are highly needed in our correctional system (Zarkin et al., 2012). To substantially reduce drug use, policymakers should consider increasing funding for drug treatment programs. This would give prisoners greater access to treatment programs and allow them to overcome substance abuse under the supervision of professionals. Overall, it would be beneficial, both for society and the criminal justice system, for the corrections system to return to the rehabilitative stance it once had towards drug abuse.
Policing policies have also affected the opioid epidemic. Police officers are normally the first public officials to come in contact with those suffering from substance abuse (Davis, Green, and Beletsky, 2017). Therefore, it’s important that local departments provide adequate training to officers so that they can effectively help those individuals. Thankfully, many departments have equipped officers with naloxone or Narcan, which is a nasal spray that reverses the effects of an opiate overdose (Davis et al., 2017). However, not all departments have provided Narcan to its officers. Additionally, not all police departments have policies that focus on helping those that suffer from substance abuse. Aggressive policing tactics and punitive laws may have exacerbated the current epidemic by discouraging individuals from seeking help when someone is suffering from an overdose (Davis et al., 2017). Of course, this leads to higher overdose deaths than a non-punitive approach to substance abuse. Further exacerbating this epidemic is the fact that many officers are unequipped or not trained to deal with substance abusers (Davis et al., 2017). These factors support the idea that other agencies beyond law enforcement may need to step in to help resolve this epidemic, and policymakers may want to view this epidemic as a public health problem, not a legal one.
Socioeconomic Problems
There are multiple factors that determine the levels of substance abuse within a society. Most of these factors relate to the political economy of local areas, particularly the levels of poverty, job opportunities, and income inequality (Gorelick, 1992). However, there are also other factors which can promote substance abuse. Factors such as a high crime rate, the presence of drug dealers, and the availability of drugs in general can also contribute to the amount of substance abuse within an area (Fishbein and Pérez, 2000). Educational attainment is also strongly related to substance abuse, and individuals that are most susceptible to substance abuse are those who have dropped out or disengaged from school (Gorelick, 1992). For example, the prevalence of substance abuse among high-school dropouts is 9.3 percent, and college dropouts have a prevalence rate of 11.2 percent (Gorelick, 1992). This is significantly higher than high-school and college graduates who have a substance abuse rate of 7.5 percent and 6.8 percent respectively (Gorelick, 1992). Substance abuse is also prevalent among racial minorities, the homeless, and those living in rural areas (Gorelick, 1992). Substance abuse is especially problematic for the homeless. One study found that the homeless population has a lifetime prevalence rate of substance abuse of 30.8 percent (Gorelick, 1992). It is important to note that none of these factors by themselves would necessarily be responsible for substance abuse but rather the interaction and combination of these factors may eventually result in substance abuse (Fishbein and Pérez, 2000). Generally, these studies show that those marginalized by society would benefit the most from drug treatment programs due to socioeconomic factors exacerbating substance abuse problems among these populations.
Sociodemographic factors can also affect the type of treatment given to patients. Researchers have found that physicians may rely on stereotypes when diagnosing patients with substance use disorder. These studies have found that doctors are more likely to diagnose patients with substance use disorder if they are non-white, have little to no education, and are of low socioeconomic status (SES) (Gorelick, 1992). These stereotypes can also apply to referrals, and are more likely to be made for patients who are African American or for those who are of low SES (Gorelick, 1992). Furthermore, these stereotypes also extend to the type of treatment programs patients are referred to. Generally, physicians are more likely to refer poor patients to government funded treatment programs, while wealthier patients are referred to privately funded treatment programs (Gorelick, 1992). Some studies have found that whites are more likely to be referred to self-help groups, and blacks are more likely to be referred to inpatient care (Gorelick, 1992). These studies show clear discrepancies in diagnosis, referral, and quality of care given to different sociodemographic groups with the most marginalized groups generally being given the worst treatment.
Sadly, most of the treatment programs that serve marginalized populations are understaffed and underfunded. This is mainly due to treatment programs competing for funding with other agencies that combat drug abuse, such as law enforcement (French, 1995). Thankfully, as Figure 4 shows, the federal government has increased spending for treatment programs over the past few years. In 2007, only $8 billion was spent on treatment while in 2016 $15 billion was spent on treatment (Figure 4). America currently spends around $30 billion dollars to combat drug abuse, and 48% is spent on treatment programs (Figure 4). However, more funding still goes toward the enforcement of drug policies rather than the treatment of drug abusers (Figure 4). As one study showed, this may be due to the lack of clear monetary benefit of treating drug offenders (French, 1995). Simply put, it is hard to see how much money these programs save. Overall, there are multiple factors, both individual and social, that determine who becomes a drug abuser and the level of care available to abusers.
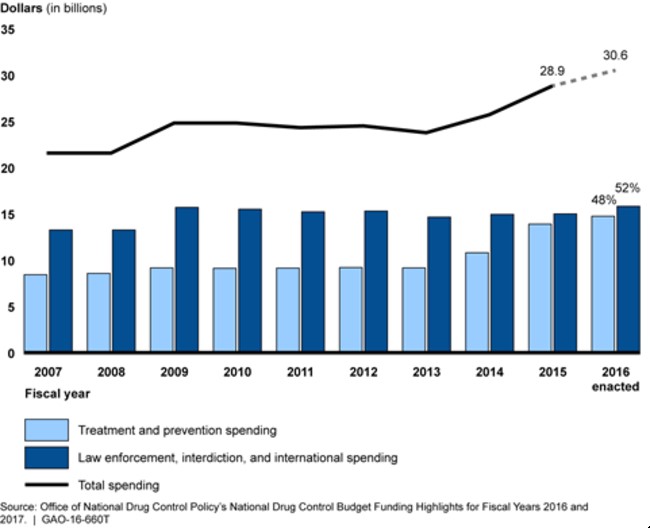
Figure 4. GAO. This figure shows the increase in federal government spending for drug treatment programs and law enforcement programs from 2007-2015. Until 2015, very few funds were allocated towards drug treatment programs with more funding being allocated towards the enforcement of drug laws instead.
Conclusion
This epidemic is the result of the interaction of various systemic problems that have persisted in this country for decades. While this paper was not entirely comprehensive in examining this epidemic, I have focused on some of the major factors that have contributed to this epidemic. First, our medical system has suffered from false advertising of prescription opioids, a lack of oversight in prescribing opioids, and the influence of corrupt pharmaceutical executives. Second, our legal system still carries with it a punitive mindset from the War on Drugs era, increasing the number of drug addicts in prison. The legal system also has been asked to resolve a public health crisis; a task which it is entirely ill-equipped to handle. Last, the social welfare agencies we rely upon to help addicts are horribly underfunded and understaffed.
The resolution of these problems will not come overnight, but leaders and researchers should collaborate and begin to implement effective strategies today before this crisis becomes uncontrollable. Effective solutions would require the input of leaders from the fields of medicine, law, and social welfare. A good starting point would be to change our view of this epidemic by seeing it as a matter of health and not of criminality. By treating this epidemic as a public health problem, more resources could be directed towards combating it, and the public could be better made aware of what they can do to help stop this epidemic. Only when America treats this crisis as a public health problem will true progress be made in resolving it.
References
Alam, A., & Juurlink, D. N. (2016). “The Prescription Opioid Epidemic: An Overview for Anesthesiologists.” Canadian Journal of Anesthesia, 63(1):61-68.
Clarke, J. L., Skoufalos, A., and Scranton, R. (2016). “The American Opioid Epidemic: Population Health Implications and Potential Solutions. Report from the National Stakeholder Panel.” Population Health Management, 19:1-7.
Clear, T. R., and Frost, N. (2014). The Punishment Imperative: The Rise and Failure of Mass Incarceration in America. New York: New York University Press.
Davis, C., Green, T., and Beletsky, L. (2017). “Action, Not Rhetoric, Needed to Reverse the Opioid Overdose Epidemic.” Journal of Law, Medicine & Ethics, 45: 20-23.
Fishbein, D. H., and Pérez, D. M. (2000). “A Regional Study of Risk Factors for Drug Abuse and Delinquency: Sex and Racial Differences.” Journal of Child & Family Studies, 9(4): 461-479.
French, M. T. (1995). “Economic Evaluation of Drug Abuse Treatment Programs: Methodology and Findings.” American Journal of Drug & Alcohol Abuse, 21(1): 111-135.
Government Accountability Office. (2016). “Progress toward Some National Drug Control Strategy Goals, but None Have Been Fully Achieved.” Retrieved Oct. 3, 2017 (https://www.gao.gov/assets/680/677235.pdf).
Gorelick, D. A. (1992). “Sociodemographic Factors in Drug Abuse Treatment.” Journal of Health Care for the Poor and Underserved, 3(1): 49.
Jonnes, J. (1995). “The Rise of the Modern Addict.” American Journal of Public Health, 85(8 Pt 1), 1157-1162.
Kanouse, A. B., and Compton, P. (2015). “The Epidemic of Prescription Opioid Abuse, the Subsequent Rising Prevalence of Heroin Use, and the Federal Response.” Journal of Pain & Palliative Care Pharmacotherapy, 29(2): 102-114.
Lembke, A. (2016). Drug Dealer, MD. Baltimore, MD: John Hopkins University Press.
Manchikanti L., Helms S. , Fellows B., Janata J., Pampati V., Grider J., and Boswell M. (2012). “Opioid Epidemic in the United States.” Pain Physician, 15: 9-38.
National Institute on Drug Abuse. 2017. “Overdose Death Rates.” Retrieved Aug. 27, 2017 (https://www.drugabuse.gov/related-topics/trends-statistics/overdose-death-rates).
Olson, D. E., and Lurigio, A. J. (2014). “The Long-Term Effects of Prison-Based Drug Treatment and Aftercare Services on Recidivism.” Journal of Offender Rehabilitation, 53(8): 600-619.
Reinl, J. (2017). “Trump Administration and the Opioid Epidemic in the USA.” The Lancet, 389(10085):2181.
The Sentencing Project. 2017. “Trends in US Corrections.” Retrieved Sep. 17, 2017 (http://sentencingproject.org/wp-content/uploads/2016/01/Trends-in-US-Corrections.pdf).
Vashishtha, D., Mittal, M. L., and Werb, D. (2017). “The North American Opioid Epidemic: Current Challenges and a Call for Treatment as Prevention.” Harm Reduction Journal, 14:1-6.
Zarkin, G. A., Cowell, A. J., Hicks, K. A., Mills, M. J., Belenko, S., Dunlap, L. J., Houser, K. A., and Keyes, V. (2012). “Benefits and Costs of Substance Abuse Treatment Programs for State Prison Inmates: Results from a lifetime simulation model.” Health Economics, 21(6): 633–652.
Acknowledgments: Special thanks to Dr. McNulty of the Department of Sociology for his help in carrying out this project.
Citation style: ASA